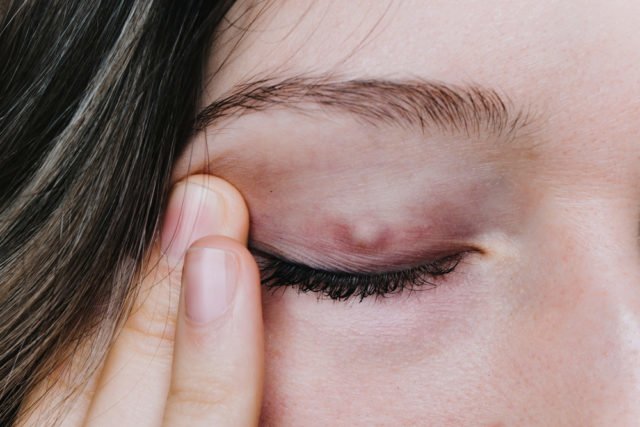
A chalazion is a small and usually painless lump or swelling which appears on the eyelid. The cause for chalazion is a blocked meibomian or oil gland. Chalazion can develop on the upper or lower eyelid and it can disappear without treatment. The term which is used to describe multiple chalazion is chalazia. There are some cases when chalazion is confused with an external or internal stye. An external stye is an infection in the area of sweat gland and eyelash follicle. An internal stye is an infection of the meibomian gland. Chalazia usually are not painful while styes are usually painful. After you have styes, then chalazia can develop. You should visit your doctor if you think that you have a chalazion, especially if you have had chalazia in the past or it blocks your vision. You should know that chalazion is not contagious. Chalazion can develop at any age and childhood is also included. In the most cases chalazion is painless but also there are some cases when the affected area can be somewhat tender to touch. This condition is very common and in the most cases it can disappear on its own without using any kind of treatment or when you just use warm compresses as your natural treatment. Patients who have untreated meibomian gland dysfunction or chronic blepharitis are having chances of developing another chalazion in the future in any of their eyelids [1]. There are some preventive measures against the development of chalazion and they include ensuring that your lid margins are clean and that the oil gland flow will remain unobstructed. The best defenses against the recurrence of this condition are the treatments of underlying MGD and blepharitis.
Symptoms of chalazion
Usually, chalazion is appearing as a painless swelling or lump on your lower or upper eyelid. Chalazia can affect both lower and upper lids and it can happen in both eyes at the same time. Depending on the location and size of your chalazion, it can blur or block your vision. It is not a common, but chalazion can be painful, swollen and red if an infection is present. Typically chalazion is healing within a few weeks but also there are some cases when it will resolve slowly over months. If scarring or infection does not develop, then there are no long – term consequences to happen and recurring chalazion are unlikely to happen.

Causes of chalazion
This condition is caused by a blockage in one of the tiny meibomian glands of the lower and upper eyelids. We know that these glands produce oil which can help to moisten our eyes. You should know that each of the meibomian glands in our eyelids is producing oil which flows out of the gland onto the eye’s surface. It is known fact that in the lower lid there are about 25 meibomian glands while in the upper lid there are about 40 – 50 meibomian glands. Meibomian glands are actually located within the tarsal plate. This is a firm tissue which is located under the skin of your lids. The oil which is produced by these glands exits from each gland through a tiny circular opening which is just behind the eyelashes of the lower and upper lids of your both eyes. When the oil in the gland becomes too thick to flow out of the gland then chalazion is caused. Also when the opening of your gland becomes obstructed, then chalazion can be also formed. The oil cannot go anywhere and it starts to build up inside of your eyelid gland and it is forming a type of meibomian cyst. This trapped oily material can have the texture of solid butter or even of hardened wax. The gland can leak, releasing the oil into the tissue of your eyelid which is causing inflammation and in some cases scar tissue. When people have recurring or unusual chalazia, then it can be a symptom of more serious condition but these chalazia are rare. [2,3]
Risk factors: This condition is most common in people who have inflammatory conditions like as long – term inflammation of the eyelid, chronic blepharitis, rosacea, acne and seborrhea. Chalazion is also common in people who have an infection covering the inside of the eyes and eyelids and people who have viral conjunctivitis [4,5].
References:
[1] American Optometric Association. Chalazion. Retrieved from www.aoa.org/healthy-eyes/eye-and-vision-conditions/chalazion?sso=y
[2] Arita R, Fukuoka S, Morishige N. New insights into the morphology and function of meibomian glands. Experimental Eye Research. 2017;163:64-71.
[3] Griff AM. Treating a chalazion at home. Medical News Today. 2019. Retrieved from www.medicalnewstoday.com/articles/324215
[4] Lee JWY, Yau GSK, Wong MYY, Yuen CYF. A comparison of intralesional triamcinolone acetonide injection for primary chalazion in children and adults. The Scientific World Journal. 2014;2014:413729.
[5] Mansour AM, Chan CC, Crawford MA, et al. Virus-induced chalazion. Eye. 2006;20(2):242-6.