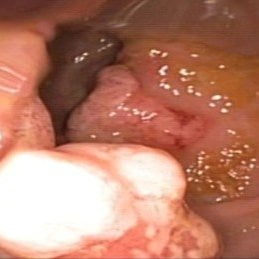
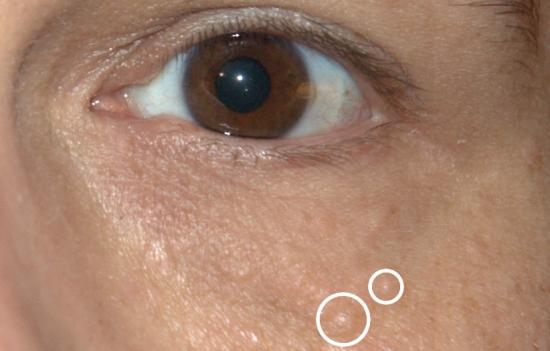
SJS – Stevens-Johnson syndrome is a rare, but serious disorder of the skin and mucous membranes. Usually, it is a reaction to medication [1,3,4,5,6] and it starts with flu-like symptoms, but it is followed by a painful rash that spreads and blisters. Then, the top layer of the affected skin dies, sheds and it begins to heal after several days. Stevens-Johnson syndrome is a medical emergency and it usually requires hospitalization.
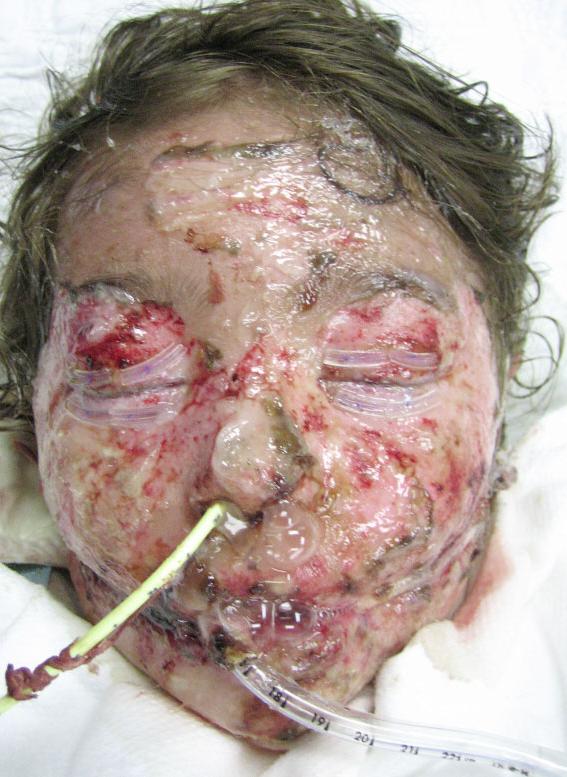
The treatment of Stevens-Johnson syndrome focuses on removing the cause, caring for wounds, controlling the pain, and minimizing the complications as the skin regrows. The affected person can take weeks to months to recover from it. TEN (toxic epidermal necrolysis) is a more severe form of this condition. This condition involves more than 30% of the skin surface and extensive damage to the mucous membranes [2]. If your Stevens-Johnson syndrome was caused by a medication, then you will need to permanently avoid that drug and others closely related to it.
Stevens-Johnson Syndrome: Symptoms
Contents
The early signs of Stevens-Johnson syndrome happen 1 – 3 days before a rash develops and they include:
- Burning eyes
- Fatigue
- A sore mouth and throat
- Fever
As the Stevens-Johnson syndrome develops, there can be other signs and symptoms, such as
- Shedding of skin within days after blisters form
- Blisters on your skin and the mucous membranes of the mouth, nose, eyes, and genitals
- A red or purplish rash that spreads
- Unexplained widespread skin pain
Stevens-Johnson syndrome needs immediate medical attention. You need to seek emergency medical care if you are experiencing signs and symptoms of this condition. The drug-induced reactions can happen during the use of a medication or up to two weeks after discontinuing it.
Stevens-Johnson Syndrome: Causes
Stevens-Johnson syndrome is a rare and unpredictable disease. In many cases, doctors cannot identify the exact cause for this condition, but usually, Stevens-Johnson syndrome is triggered by infection, medication, or both. You can react to medication while you are using it or up to two weeks after you have stopped using it. The most common drugs which cause Stevens-Johnson syndrome are next:
- Pain relievers, such as naproxen sodium (Aleve), ibuprofen (Advil, Motrin IB, others), acetaminophen (Tylenol, others) [3,4]
- Nevirapine (Viramune, Viramune XR) [5]
- Antibacterial sulfonamides (including sulfasalazine) [1]
- Medications to treat seizures and mental illness (anticonvulsants and antipsychotics) [6]
- Antigout medications, such as allopurinol
HIV and pneumonia are infections that can cause Stevens-Johnson syndrome. [7]
Risk factors
There are some factors that can increase your risk for Stevens-Johnson syndrome, such as
- Genetic factors: If you have certain genetic variations, then this can increase your risk for Stevens-Johnson syndrome, especially if you are taking drugs for seizures, gout, or mental illness. [6]
- An HIV infection: It is noticed that among people with HIV, the incidence of Stevens-Johnson syndrome is about 100 times greater than among the general population. [7]
- A family history of Steven – Johnson syndrome: If you have an immediate family member who has had Stevens-Johnson syndrome, then you have increased chances of developing it.
- Cancer: It is noticed that people who have cancer, especially blood cancer, have increased chances of developing Stevens-Johnson syndrome. [8]
- A weakened immune system: The immune system can be affected by autoimmune diseases, HIV/AIDs, and an organ transplant. [9]
Complications
The most common complications caused by Stevens-Johnson syndrome include:
- Permanent skin damage: Your skin may have abnormal bumps and coloring when it grows back following Stevens-Johnson syndrome. Also, you can have scars. Lasting skin problems can cause your fingernails and toenails not to grow normally and your hair to fall out. [2]
- Lung involvement: The Stevens-Johnson syndrome can lead to acute respiratory failure.
- Eye problems: It is noticed that the rash caused by Stevens-Johnson syndrome can lead to eye inflammation, light sensitivity, and dry eye. When it is a severe case, then it can lead to visual impairment and in rare cases blindness.
- Blood infection (sepsis): Sepsis is happening when the bacteria from an infection enter your bloodstream and spreads throughout your body. Sepsis is a rapidly progressing and life-threatening condition, that could lead to organ failure and shock. [10]
References:
[1] Mawson AR, Eriator I, Karre S. Stevens-Johnson syndrome and toxic epidermal necrolysis (SJS/TEN): Could retinoids play a causative role? Medical Science Monitor. 2015;21:133-43.
[2] Cohen V. Toxic epidermal necrolysis (TEN). 2018. Retrieved from emedicine.medscape.com/article/229698-overview
[3] U.S. Food & Drug Administration (FDA). FDA Drug Safety Communication: FDA warns of rare but serious skin reactions with the pain reliever/fever reducer acetaminophen. Retrieved from www.fda.gov/drugs/drug-safety-and-availability/fda-drug-safety-communication-fda-warns-rare-serious-skin-reactions-pain-relieverfever-reducer
[4] Lebrun-Vignes B, Guy C, Jean-Pastor MJ, et al. Is acetaminophen associated with a risk of Stevens–Johnson syndrome and toxic epidermal necrolysis? Analysis of the French Pharmacovigilance Database. British Journal of Clinical Pharmacology. 2018;84(2):331-8.
[5] Namayanja GK, Nankya JM, Byamugisha JK, et al. Stevens – Johnson syndrome due to nevirapine. African Health Sciences. 2005;5(4):338–40.
[6] Kaniwa N, Sugiyama E, Saito Y, et al. Specific HLA types are associated with antiepileptic drug-induced Stevens-Johnson syndrome and toxic epidermal necrolysis in Japanese subjects. Pharmacogenomics. 2013;14(15):1821-31. doi:10.2217/pgs.13.180.
[7] Knight L, Muloiwa R, Dlamini S, Lehloenya RJ. Factors associated with increased mortality in a predominantly HIV-infected population with Stevens Johnson syndrome and toxic epidermal necrolysis. PLoS One. 2014;9(4):e93543. doi:10.1371/journal.pone.0093543
[8] Ng CY, Chen CB, Wu MY, et al. Anticancer drugs induced severe adverse cutaneous drug reactions: An updated review on the risks associated with anticancer targeted therapy or immunotherapies. Journal of Immunology Research. 2018.
[9] Abe R. Immunological response in Stevens–Johnson syndrome and toxic epidermal necrolysis. The Journal of Dermatology. Special Issue: Special Issue: Pemphigus updates from around the world (pages 1‐41). 2015;42(1):42-8.
[10] Harnar TJ, Dobke M, Simoni J, Ninnemann JL. Toxic epidermal necrolysis complicated by severe wound sepsis: a case study. Journal of Burn Care & Rehabilitation. 1987;8(6):554-7.