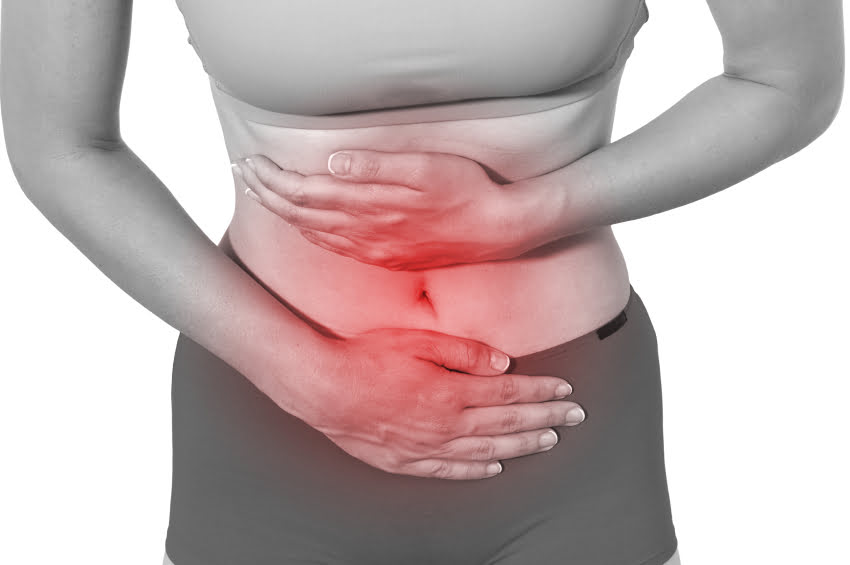
Dysmenorrhea is very common for girls to have mild pain with their periods a couple of days each month. But if their pain is not relived when they use over – the – counter pain medicine and they cannot do their everyday activities, then they may have dysmenorrhea. This condition can be said that it is difficult monthly flow. It is very normal for women to have abdominal cramps on the first day or two of their period, but about 10% of women experience severe pain [1].
Symptoms and complications of Dysmenorrhea:
Contents
The pain is the main symptom of dysmenorrhea. This is happening in the lower abdomen during menstruation and also it can be felt in your thighs, lower back and hips. Also there are other symptoms which include lightheadedness, diarrhea, vomiting, nausea and general achiness. For most women, this pain usually starts shortly before or during their menstrual periods, peaks after 24 hours and it subsides after two to three days. There are some cases in which pieces or clots of bloody tissue from the lining of the uterus are expelled from the uterus and they are causing pain. This condition can be congestive (deep, dull ache) or spasmodic (sharp pelvic cramps at the start of menstrual flow). It is known fact that the symptoms of the secondary dysmenorrhea can start sooner in the menstrual cycle compared to symptoms of the primary dysmenorrhea and they usually last longer. If you have painful periods, then you should talk with your doctor to check if you have some underlying disorder that is causing the secondary dysmenorrhea. Your doctor can check your urine and blood and you may be given a pelvic examination. Also your doctor may want to make an ultrasound to get a picture of your internal organs. Also he can use the technique of laparoscopy for a direct look into the uterus.
Causes for dysmenorrhea
It is thought that the primary dysmenorrhea is caused by the excessive levels of the prostaglandins which are hormones that are making the uterus contract during the menstruation and childbirth. The pain probably results from the contractions of the uterus which happen when the blood supply to the endometrium (its lining) is reduced.

Also there are factors which can make the pain of the primary dysmenorrhea even worse such as starting menstruating before age 11, being overweight, drinking alcohol, smoking, psychological or social stress, lack of exercise and a uterus that tilts backwards (retroverted uterus) instead of forward. There are many conditions which can cause the secondary dysmenorrhea such as
- The use of intrauterine device (IUD), a birth control method [2]
- An ovarian cyst or tumor [3]
- PID (pelvic inflammatory disease. This is primarily an infection of the fallopian tubes, but can also affect the ovaries, uterus and cervix [4]
- Endometriosis, they are fragments of the endometrial lining which are found on other pelvic organs [5]
- STI (sexually transmitted infection) [6]
- Adenomyosis, which is the tissue that lines the uterus (called the endometrium) begins to grow within its muscular walls [5]
- Fibroids – benign tumors that develop within the uterine wall or are attached to it [7]
Types of dysmenorrhea:
- Primary dysmenorrhea: This is a menstrual pain which is not a symptom of an underlying gynecologic disorder but it is related to the normal process of the menstruation. The most common type is the primary dysmenorrhea and it is affecting more than 50% of women and it is quite severe in about 15%. This type is more affecting girls during adolescence. For many women, this problem eases as they mature which is usually happening after the pregnancy. This is painful condition and in some cases it can be debilitating for brief periods of time but it is not harmful.
- Secondary dysmenorrhea: This type of menstrual pain is generally related to some kind of gynecologic disorder. Most of these disorders can be easily treated with some kinds of medications or surgery. This type of dysmenorrhea is affecting women during adulthood at most.
References:
[1] Yesuf TA, Eshete NA, Sisay EA. Dysmenorrhea among University Health science students, Northern Ethiopia: Impact and associated factors. International Journal of Reproductive Medicine. 2018.
[2] Shahnazi M, Sarrafi S, Jafarabadi MA, et al. Comparing hemorrhages and dysmenorrhea with copper T380A and multiload 375 intrauterine devices: A randomized clinical trial. Journal of Caring Sciences. 2014;3(3):193–204.
[3] Jeong JY, Kim MK, Lee I, et al. Polycystic ovarian morphology is associated with primary dysmenorrhea in young Korean women. Obstetrics & Gynecology Science. 2019;62(5):329–34.
[4] Tai FW, Chang CYY, Chiang JH, et al. Association of pelvic inflammatory disease with risk of endometriosis: A nationwide cohort study involving 141,460 individuals. Journal of Clinical Medicine. 2018;7(11):379.
[5] Bernardi M, Lazzeri L, Perelli F, et al. Dysmenorrhea and related disorders. F1000 Research. 2017;6:1645.
[6] University of Oxford. Undiagnosed STIs can increase negative PMS symptoms: Women’s menstrual cycles can directly affect their general health. Science Daily. 2018. Retrieved from www.sciencedaily.com/releases/2018/09/180917111535.htm
[7] Khyade RL. A study of menstrual disturbance in cases of fibroid uterus. International Journal of Reproduction, Contraception, Obstetrics and Gynecology. 2017;6(6).