Epididymitis is an inflammation of the coiled tube (known as epididymis) at the back of the testicle which stores and carries sperm. It is known that males of any age can get epididymitis. This condition is most often caused by a bacterial infection, including STIs (sexually transmitted infections), such as Chlamydia or gonorrhea [1]. In some cases, a testicle becomes inflamed, a condition called epididymo – orchitis. You should practice safer sex, so in this way you will help to protect against STIs which can cause epididymitis. If you have recurrent urinary tract infections or other risk factors for epididymitis, then your doctor can recommend you to discuss about other ways of preventing a recurring.
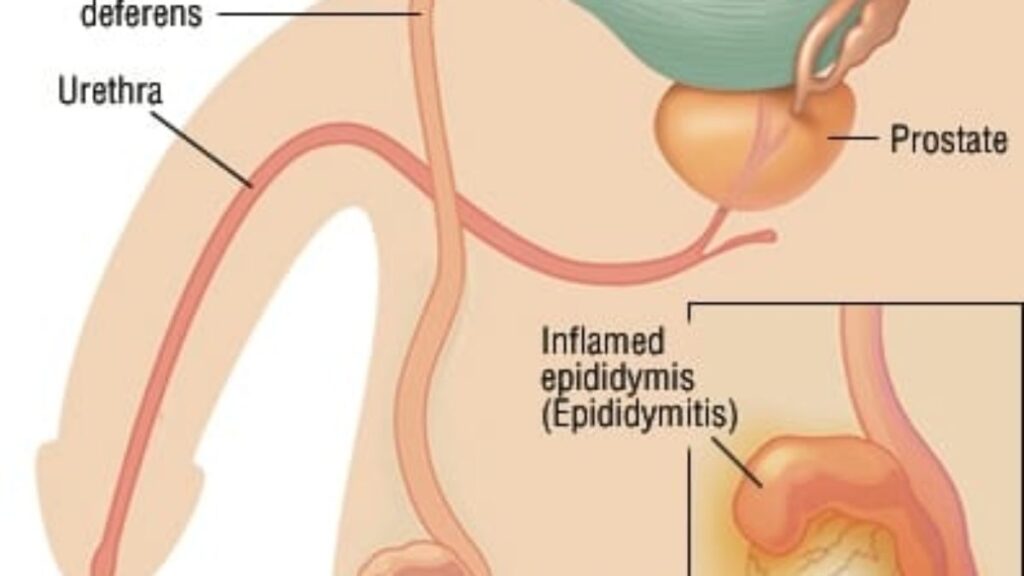
Epididymitis Symptoms
The most common signs and symptoms of epididymitis include:
- Less commonly, fever
- Blood in the semen
- Pain or discomfort in the lower abdomen or pelvic area
- Discharge from the penis
- A painful urination or an urgent or frequent need to urinate
- A testicle pain and tenderness, usually on one side, that usually comes on gradually
- A swollen, red or warm scrotum
Chronic epididymitis: The epididymitis which lasts longer than 6 weeks or that recurs is considered chronic. The symptoms of chronic epididymitis might come on gradually and the cause of chronic it is not identified. You should never ignore scrotal pain or swelling, which can be caused by a number of conditions. Some of these conditions require immediate treatment to avoid permanent damage. If the scrotal pain is severe, then you should seek emergency medical treatment. You should see a doctor if you have a discharge from your penis or pain when you urinate. Your doctor will check for enlarged lymph nodes in your groin and an enlarged testicle on the affected side. [2]
Also, your doctor can make a rectal examination to check for prostate enlargement or tenderness. There are some tests, which your doctor can recommend, such as ultrasound, urine and blood tests, STI screening. If an abscess has formed, then your doctor might make you surgery to drain it. In some cases, all parts of the epididymis need to be removed surgically. Also, if the epididymitis is caused by underlying physical abnormalities, you may have to go to surgery. You should tell your doctor all the symptoms that you have and how long they last. If you take some vitamins, supplements or medications, then tell your doctor and include the doses of them. If you had previous STIs, tell your doctor.
Epididymitis Causes
The most common causes for epididymitis include:
- Tuberculosis: In rare cases, this can be caused by tuberculosis infection. [3]
- Trauma: The groin injury can lead to epididymitis.
- Urine in the epididymis (known as chemical epididymitis): This condition is happening when the urine flows backward into the epididymis, possibly because of heavy lifting or straining. [4]
- Other infections: The prostate infection or bacteria from a urinary tract might spread from the infected site to the epididymis. Also, the viral infections, such as mumps virus, could lead to epididymitis.
- STIs: The Chlamydia and gonorrhea are the most common causes of epididymitis in young and sexually active men. [1]
Risk factors
There are some behaviors which could lead to STIs and they put you at risk for sexually transmitted epididymitis, including having [1]:
- A history of STIs
- Sex without a condom
- Sex with a partner who has a STI
Also, there are some risk factors for nonsexually transmitted epididymitis, such as
- A prostate enlargement, which increases the risk of bladder infections and epididymitis [5]
- An uncircumcised penis or an anatomical abnormality of the urinary tract
- A history of medical procedures that affect the urinary tract, such as insertion of a urinary catheter or scope into the penis [4]
- History of prostate or urinary tract infections [4,5]
Complications
Here are the most common complications caused by epididymitis:
- The epididymo – orchitis, if the condition spreads from your epididymis to your testicle
- A pus – filled infection (also known as abscess) in the scrotum
- In rare cases, reduced fertility
References:
[1] Venkateshwaran S, Azraan A, Ruslan A, et al. Epididymitis and its aetiologies in a central London sexual health clinic. 2020;32(1):96-9.
[2] Nickel C. Chronic Epididymitis: A practical approach to understanding and managing a difficult urologic enigma. Reviews in Urology. 2003;5(4):209–15.
[3] Borges WM, Bechara GR, de Miranda MML, et al. Epididymis tuberculosis: Case report and brief review of the literature. Urology Case Reports. 2019;26:100969.
[4] Lynch S. Acute epididymitis. Journal of the American Academy of Physician Assistants. 2018;31(3):50-1.
[5] Zhang J, Dong M, Hu X, et al. Prostatic adenocarcinoma presenting with metastases to the testis and epididymis: A case report. Oncology Letters. 2016;11(1):792-4.




