The impetigo is an infection of the skin. When it affects just the surface, then it is known as superficial impetigo. Childhood impetigo is also known as school sores, because it is a very common condition among school children. The sores of the skin which are caused by the impetigo are usually itchy. Also, impetigo can affect deeper parts of the skin which is known as ecthyma. This condition can happen on healthy skin. But, also it can happen where the skin was injured by a scrape, cut or insect bite. The impetigo is most common condition among children aged 2 – 5. The impetigo is contagious, which means that it is easily passed from one person to another. [1,2]
Also, the childhood impetigo can be spread around a household. Children can infect their parents and other family members and they can re-infect themselves. The sores may start out as blisters which burst and they become weepy, before they are covered with a crust. Usually, the impetigo is not a serious infection and it should clear up in a period of few days after starting medical treatment. Children that are affected by the childhood impetigo are very infectious (contagious), but the spread of impetigo can be reduced by practicing good hygiene, covering the sores with dressings and you should keep away your child away from other children until they are no longer infectious. [2]
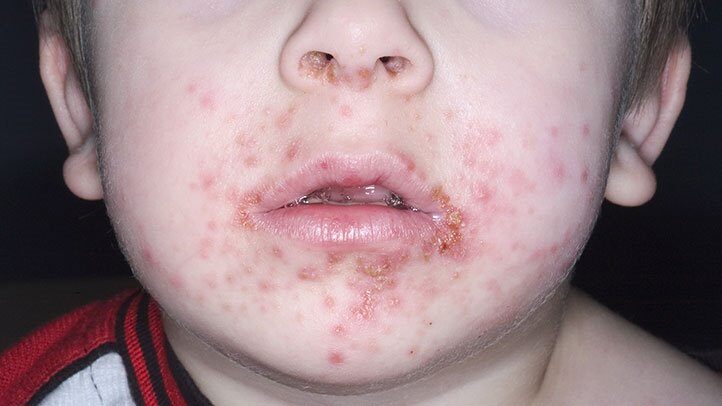
Childhood impetigo symptoms
Contents
The symptoms of childhood impetigo can occur a bit differently in each child. Also, the symptoms vary depending on which bacteria caused it. The symptoms of childhood impetigo:
- Swelling of nearby lymph glands (nodes)
- Red bumps
- Areas that are red, swollen and may itch
- Sores that are filled with fluid, draining fluid, or crusted over
The sores or bumps can be painful and they can appear anywhere on the body. Most commonly, they happen on legs, arms and face. The symptoms of childhood impetigo can be like other health conditions. In many cases parents are worried about this condition, because it can look quite serious, but usually it is a mild infection which is easy to treat. You should see the doctor of your child, so you will be sure if your child has childhood impetigo. He or she will ask about the symptoms of your child and health history.
He or she will give your child a physical exam and a sample of the pus from the sores will be sent to a lab. This is known as a culture and it is done to see what type of bacteria is cause for the childhood impetigo.
Childhood impetigo causes
The childhood impetigo is caused by bacteria. The bacteria which can cause childhood impetigo include:
- Staphylococcus aureus [2]
- Group A beta – hemolytic streptococcus [3]
The mentioned bacteria can live in the nose, in the throat, on the skin, or on other part of the body without causing a problem, but there are some cases when they can cause an infection, such as the childhood impetigo. Impetigo can happen on healthy skin, but usually it happens on the skin which has been already damaged by a bite, scratch or a disease that is affecting the skin, such as chickenpox or eczema. The contact with the sore or with things which have been on the sore (such as towels, dressings, clothing) can spread infection to other people.
The impetigo is very easily spread, usually through contact with the fluid or crusts of an impetigo, which contain the bacteria. The sore takes about 1 – 3 days to develop after contact with fluid or crusts from a sore. The sore is itchy and children can scratch it, so they can spread the infection to nearby skin or other parts of their own body. The sore can be infectious for as long as it is weeping. Usually, it stops being infectious about 24 hours after starting antibiotic treatment, once it has begun to heal.
Childhood impetigo risk factors
There are many studies in which are shown that impetigo is most common in children, but also adults can have this infection [1,2]. A child has more chances of getting impetigo if he or she:
- Has other skin conditions, such as eczema or scabies [4]
- Has close contact with to others with impetigo
- Is in warm, moist (humid) air [5]
- Does not keep clean (poor hygiene) [5]
References:
[1] Hall D, Blumberg RW, Moody MD. Studies in children with impetigo: Bacteriology, serology, and incidence of glomerulonephritis. The American Journal of Diseases of Children. 1973;125(6):800-6. doi:10.1001/archpedi.1973.04160060014003
[2] Lewis LS. Impetigo. Medscape: Pediatrics: General Medicine. 2019. Retrieved from emedicine.medscape.com/article/965254-overview
[3] Bowen AC, Tong SYC, Chatfield MD, Carapetis JR. The microbiology of impetigo in Indigenous children: associations between Streptococcus pyogenes, Staphylococcus aureus,scabies, and nasal carriage. BMC Infectious Diseases. 2014;14.
[4] Kanchongkittiphon W, Gaffin JM, Phipatanakul W. Child with atopic dermatitis. Annals of Allergy, Asthma & Immunology. 2015;114(1):6–11. doi:10.1016/j.anai.2014.08.016
[5] Panesar P, Green E. Case-based learning: Impetigo. The Pharmaceutical Journal. 2020.