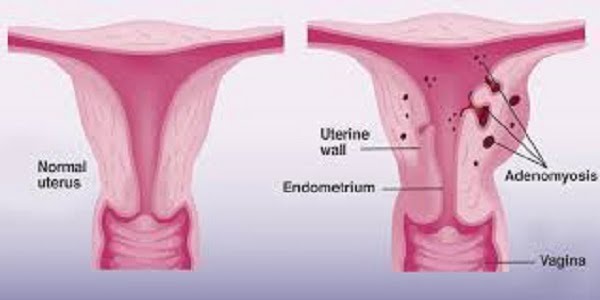
The adenomyosis is happening when the tissue which normally lines in the uterus (also known as endometrial tissue) grows into the muscular wall of the uterus. The displaced tissue is continuing to act normally (this means thickening, breaking down and bleeding) during each menstrual cycle. The enlarged uterus and painful, heavy periods can be results of this. The cause for the adenomyosis is not known, but this disease usually is resolving after menopause. For those women who have severe discomfort caused by it, hormonal treatments can help. The removal of uterus (also known as hysterectomy) can cure adenomyosis [1].
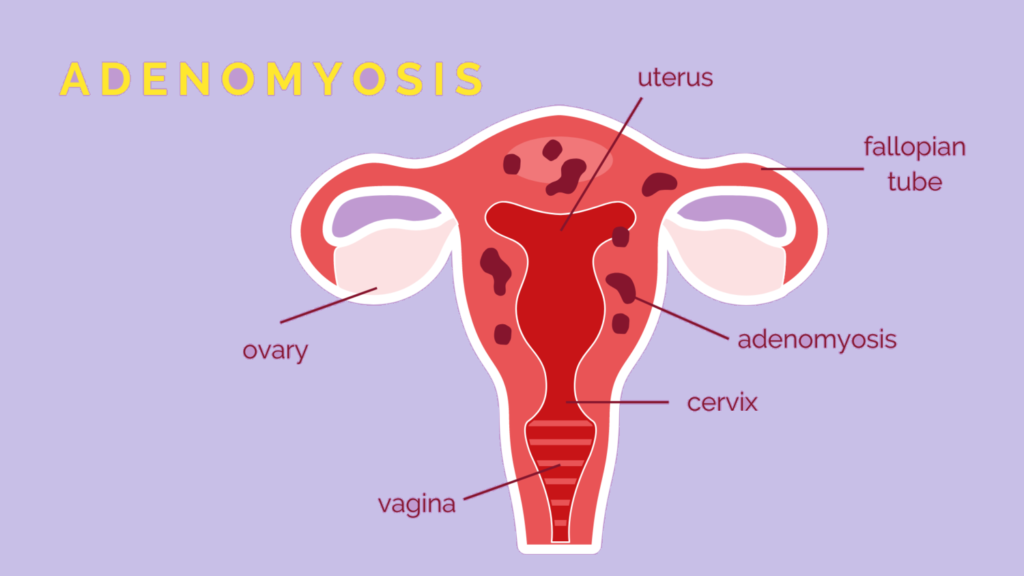
Adenomyosis Symptoms
There are some cases when adenomyosis is not causing signs or symptoms or it can cause only mild discomfort. But, the adenomyosis can cause [2]:
- Chronic pelvic pain
- You can have severe cramping or sharp, knifelike pelvic pain during menstruation (dysmenorrhea)
- Heavy or prolonged menstrual bleeding
It is known that the uterus might get bigger. You might not know if your uterus is enlarged, but you can notice that your lower abdomen feels tender or it causes pelvic pressure. It is very important to make an appointment with your doctor if you have prolonged, heavy bleeding or severe cramping during your periods which is interfering with your regular activities.
Your doctor may suspect adenomyosis based on magnetic resonance imaging of the uterus, ultrasound imaging of the uterus, a pelvic exam that reveals an enlarged, tender uterus and most important, depending on your symptoms. There are some cases when your doctor can collect a sample of uterine tissue for testing to verify that the abnormal uterine bleeding is not associated with another serious condition. But the endometrial biopsy will not help your doctor to confirm if you really suffer from adenomyosis.
Adenomyosis Causes
The cause for adenomyosis is not known. There are different theories which can explain the cause for adenomyosis, such as
- Stem cell origins: There was a recent theory in which is said that the bone marrow stem cells can invade the uterine muscle which is causing adenomyosis. [1]
- Developmental origins: There are some doctors who believe that It originates within the uterine muscle from the endometrial tissue which is deposited when the uterus is firstly formed in the fetus. [3]
- Uterine inflammation related to childbirth: In one theory is suggested that there is a link between adenomyosis and childbirth. The inflammation of the uterine lining during the postpartum period might cause a break in the normal boundary of cells which line the uterus. Also, surgical procedures on the uterus can have a similar effect. [4]
- Invasive tissue growth: There are some experts who believe that it is resulting from the direct invasion of endometrial cells from the lining of the uterus into the muscle which forms the uterine walls. The uterine incisions which are made during an operation, such as C – section (cesarean section) might promote the direct invasion of the endometrial cells into the wall of the uterus.
No matter how adenomyosis develops, its growth depends on the circulating estrogen in the women’s bodies.
Risk factors
Here are some factors which can increase your risk of getting adenomyosis:
- Middle age [5]
- Prior uterine surgery, such as a C – section or fibroid removal
- Childbirth [4]
The most cases of adenomyosis, which depends on the estrogen, are found in women who are in their 40s and 50s. The adenomyosis in these women can relate to longer exposure to estrogen compared with that of younger women. But, in the last studies was said that this condition might be common in younger women. [5]
Complications
If you often have prolonged and heavy bleeding during your periods, then you can develop chronic anemia which is causing fatigue and other health problems. It is not harmful, but the pain and excessive bleeding are associated with it can disrupt your life. You may avoid activities in which you have enjoyed in your past because you are in pain or you worry that you might start bleeding.
References:
[1] Li JJ, Chung JPW, Wang S, et al. The investigation and management of adenomyosis in women who wish to improve or preserve fertility. BioMed Research International: Uterine Fibroids: From Molecular Oncology to Reproduction. 2018.
[2] Vannuccini S, Petraglia F. Recent advances in understanding and managing adenomyosis. F1000 Research. 2019;8:F1000 Faculty Rev-283. doi:10.12688/f1000research.17242.1
[3] Jiang C, Cheng Z. Update of recent studies of adenomyosis-associated dysmenorrhea. Gynecology and Minimally Invasive Therapy. 2016;5(4):137-40.
[4] Tamura H, Kishi H, Asai-Sato M, et al. Complications and outcomes of pregnant women with adenomyosis in Japan. Reproductive Medicine and Biology. 2017;16(4):330–6. doi:10.1002/rmb2.12050
[5] Protopapas A, Grimbizis G, Athanasiou S, Loutradis D. Adenomyosis: Disease, uterine aging process leading to symptoms, or both? Facts, Views and Vision in Obstetrics and Gynaecology. 2020;12(2):91–104.