The porokeratosis is a rare skin disorder which is affecting fewer than 200,000 Americans. Typically, it presents as small, round patch on the skin which have a thin and raised border. This condition is usually benign, but a small number of people can develop skin cancer within a lesion. The porokeratosis was first identified in 1893 by Italian doctors Respighi and Mibelli [1]. Since then, several variations of this disease have been identified. The six main subtypes are:
- PP (punctuate porokeratosis)
- LP (linear porokeratosis)
- PPPD (porokeratosis Palmaris et plantaris disseminata, or also known as porokeratosis of Mantoux)
- DSAP (disseminated superficial actinic porokeratosis)
- DSP (disseminated superficial porokeratosis)
- PM (classic Mibelli porokeratosis)
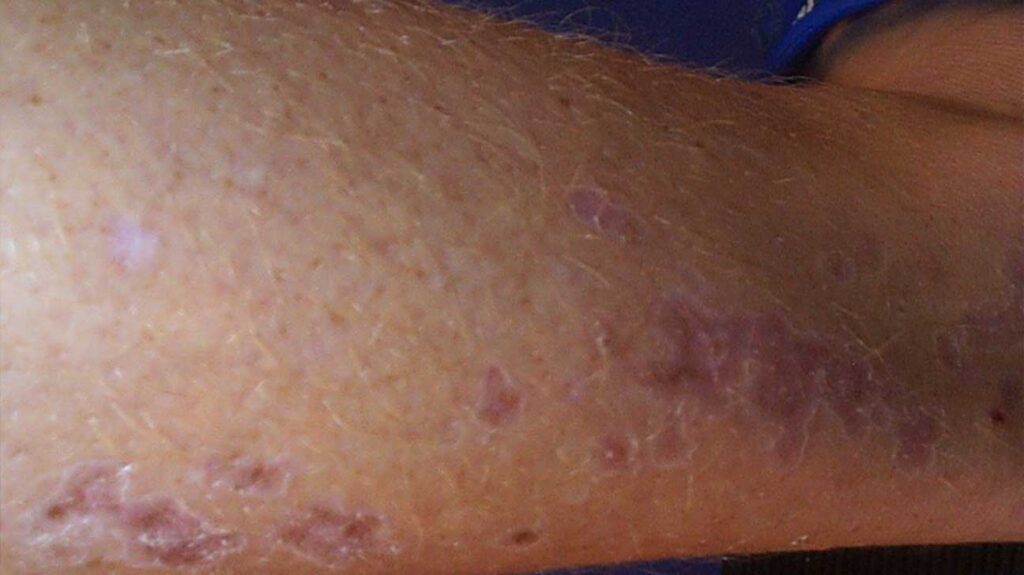
Porokeratosis Causes
The exact cause for porokeratosis is not know, but there are some factors which can make you more prone of porokeratosis, such as
- Long – term use of systemic corticosteroids
- Autoimmune and inflammatory diseases, including rheumatoid arthritis, diabetes and psoriasis [2]
- Trauma
- Burns and infections
- Suppressed immune system
- Exposure to UV radiation [3]
- Genetic defects [4]
Porokeratosis Risk factors
There are some factors which can increase your risk of getting porokeratosis, such as
- Age: It is noticed that certain types develop in children (like LP, DSP and PM), young adults (PPPD), or adults (DSAP).
- Gender: It is noticed that men have two times more chances of getting PM compared to women. On the other hand, women have more chances of getting DSAP.
- Skin color: It is noticed that fair – skinned people have more chances of getting porokeratosis.
- Genes: If some of your parents have porokeratosis, then you may inherit the damaged gene linked to the disease and develop the same type of porokeratosis. [4]
Also, you have more risk of getting porokeratosis if you are regularly exposed to direct sunlight. DSAP is the most common type of porokeratosis and it affects areas of the body that are exposed to sunlight. In one study was found that artificial sunlight has produced DSAP lesions [5].
Porokeratosis Types
There are six main subtypes of porokeratosis:
- PM (Classic Mibelli porokeratosis): It is small brownish bump which increase in size over time. They have a prominent border with a thin ridge, which means that these edges are easily identified and the bumps are slightly raised. Usually, they appear on a limb, but they can develop anywhere. It is the second most common subtype. Usually, it affects children between 5 and 10. It is not known which gender has more risk of getting it. The PM does not have any clear triggers.
- DSP (disseminated superficial porokeratosis): It is brown lesion that develop over a wide area of skin and it can develop anywhere on the body. It is very rare subtype and it typically affects adults in their 30s and 40s. Women have two times more chances of getting this subtype compared to men. The DSP has a genetic component and it results from extensive sun exposure, radiation therapy and electron beam therapy.
- PPPD (porokeratosis Palmaris et plantaris disseminata): This subtype features many small, uniform lesions which are typically the color of the skin. Usually, these lesions have little to no border. Usually, it affects the palms and soles. It is a rare subtype of porokeratosis. Usually, it affects people in their late teens and early 20s, but it can develop later in life. Men have two times more chances of being affected by this subtype. The PPPD does not have any clear triggers. [6]
- LP (linear porokeratosis): This subtype features many small and uniform reddish – brown lesions which arrange in lines along a limb or one side of the trunk. Primarily, it affects the palms and soles. The linear porokeratosis is a rare subtype. Usually, this subtype begins in infancy or early childhood. Women have more chances of getting linear porokeratosis compared to men. The linear porokeratosis does not have any clear triggers.
- PP (punctuate porokeratosis): This subtype is characterized by small lesions that look like seeds. Typically, they have a thin outer edge. Primarily, it affects the palms and soles. It is a rare subtype of porokeratosis and typically, it develops during adulthood. There is not known fact which gender is more affected. You can develop punctuate porokeratosis if you are already affected by another form of porokeratosis.
References:
[1] Mehta V, Balachandran C. Simultaneous co-occurrence of porokeratosis of mibelli with disseminated superficial actinic porokeratosis. Indian Journal of Dermatology. 2009;54(4):390–1.
doi:10.4103/0019-5154.57625
[2] Yalcin B, Uysal PI, Kadan E, Bozdoğan O. Eruptive disseminated porokeratosis in a patient with type 2 diabetes mellitus. The American Journal of Dermatopathology. 2016;38(8):e125-7. doi:10.1097/DAD.0000000000000553.
[3] Vargas-Mora P, Morgado-Carrasco D, Fustà-Novell X. Porokeratosis: A review of its pathophysiology, clinical manifestations, diagnosis, and treatment poroqueratosis. Revisión de su etiopatogenia, manifestaciones clínicas, diagnóstico y tratamiento. Actas Dermo-Sifiliográficas (English Edition). 2020;111(7):545-60.
[4] BGI Shenzhen. Scientists discover mutations associated with skin disorder (DSAP). Science Daily. 2012. Retrieved from www.sciencedaily.com/releases/2012/09/120916160931.htm
[5] Neumann RA, Knobler RM, Jurecka W, Gebhart W. Disseminated superficial actinic porokeratosis: experimental induction and exacerbation of skin lesions. Journal of the American Academy of Dermatology. 1989;21(6):1182-8. doi:10.1016/s0190-9622(89)70326-1.
[6] Irisawa R, Yamazaki M, Yamamoto T, Tsuboi R. A case of porokeratosis plantaris palmaris et disseminata and literature review. Dermatology Online Journal. 2012;18(8).




