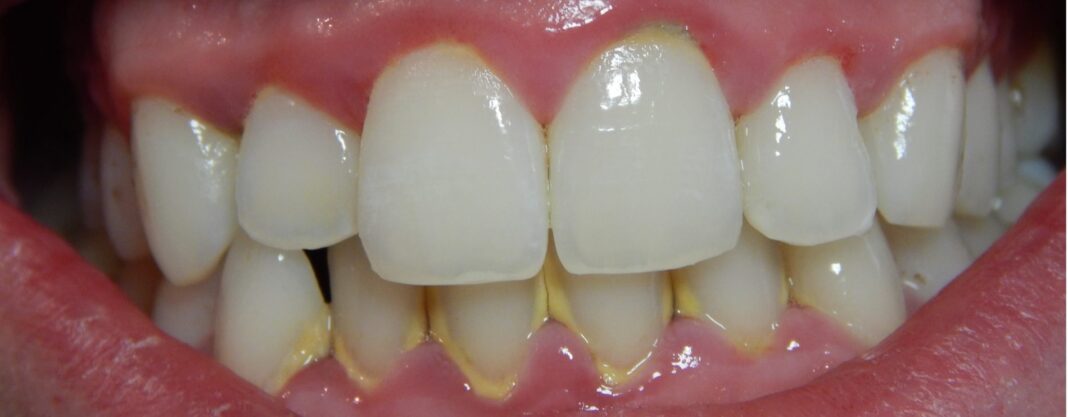
Gingivitis is a mild and common form of gum disease (known as periodontal disease) which causes swelling (inflammation), redness and irritation of your gingiva, which is the part of your gum around the base of your teeth. It is very important to take gingivitis seriously and treat it promptly. This condition can lead to much more serious gum disease, which is known as periodontitis and it can cause tooth loss.
The poor oral hygiene is the most common cause for gingivitis. The good oral hygiene, such as brushing teeth at least two times per day, flossing daily and getting regular dental checkups, can help to prevent and reverse gingivitis. [1]
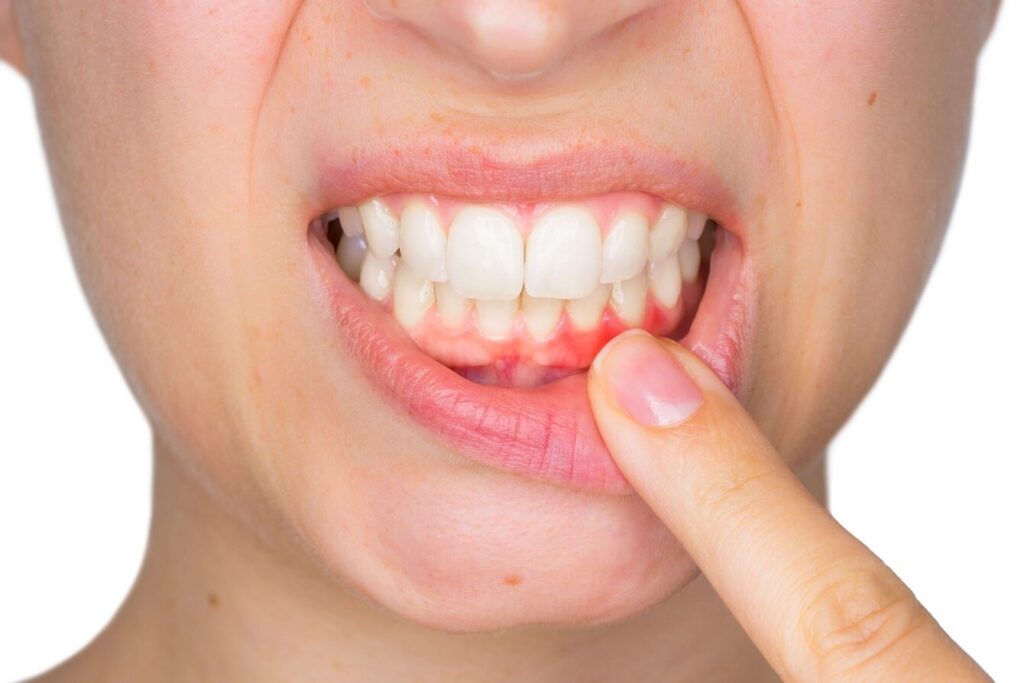
Gingivitis Symptoms
Healthy gums are firm and pale pink. They are fitted tightly around the teeth. The most common signs and symptoms of gingivitis include [1]:
- Tender gums
- Receding gums
- Bad breath
- Gums which can bleed easily when you brush or floss
- Dusky red or dark red gums
- Swollen or puffy gums
If you notice any signs and symptoms of gingivitis, then you should make an appointment with your dentist. It is very important to seek medical help in the early stages of this condition, so you will reverse your chances of damage caused by gingivitis and preventing its progression to periodontitis.
Gingivitis Causes
The poor oral hygiene is the most common cause for gingivitis and it encourages plaque to form on teeth, causing inflammation of the surrounding gum tissues. Below are given ways how plaque can lead to gingivitis:
- A plaque is forming on your teeth: The plaque is invisible and sticky film composed mainly of bacteria that forms on your teeth when sugar and starches in food interact with bacteria normally found in your mouth. The plaque needs daily removal because it re – forms quickly. [2]
- Plaque turns into tartar: The plaque which stays on your teeth can harden under your gumline into tartar (also known as calculus) which collects bacteria. Tartar is making plaque more difficult to remove, creates a protective shield for bacteria and causes irritation along the gumline. You need professional dental cleaning to remove tartar.
- Gingiva becomes inflamed (gingivitis): The longer plaque and tartar remain on your teeth, the more they will irritate the gingival, which is a part of your gum around the base of your teeth, causing inflammation. In this time, your gums will become swollen and bleed easily. The tooth decay (also known as dental caries) can also happen. If it is not treated, gingivitis can lead to periodontitis and eventual tooth loss.
Risk factors
It is very common condition and every single person can develop it. Some factors can increase your risk for gingivitis, such as
- Some medical conditions, such as certain viral and fungal infections [3]
- Genetics [4]
- Some hormonal changes, such as those related to pregnancy, menstrual cycle or use of birth control pills [5]
- Some types of drugs, such as some calcium channel blockers that are used for angina, high blood pressure and other conditions and drugs like phenytoin (like Dilantin, Phenytek) for epileptic seizures
- Conditions that decrease immunity, such as cancer treatment, HIV/AIDS or leukemia [6]
- Dental restorations that do not fit properly or crooked teeth that are difficult to clean [7]
- Poor nutrition, including Vitamin D deficiency [8]
- Dry mouth [9]
- Older age
- Smoking or chewing tobacco [10]
- Poor oral care habits [1]
Complications
It is known that the untreated gingivitis can progress to gum disease which spreads to underlying tissue and bone (also known as periodontitis), which is a much more serious condition that can lead to tooth loss. The chronic gingiva inflammation has been thought to be associated with some systemic diseases, such as rheumatoid arthritis, stroke, coronary artery disease, diabetes and respiratory disease.
In some studies are found that the bacteria responsible for peridontitis can enter your bloodstream through gum tissue, possibly affecting your lungs, heart and other parts of your body. But, a lot more studies need to be done in future to approve or disapprove this link. NUG (necrotizing ulcerative gingivitis), which is also known as trench mouth, is a severe form of gingivitis, which is causing bleeding, painful and infected gums and ulcerations.
References:
[1] Coventry J, Griffiths G, Scully C, Tonetti M. Periodontal disease. BMJ. 2000;321(7252):36–9. doi:10.1136/bmj.321.7252.36
[2] Trombelli L, Farina R, Silva CO, Tatakis DN. Plaque‐induced gingivitis: Case definition and diagnostic considerations. Journal of Periodontology. 2018;89(1):S46-S73.
[3] Yalamanchili PS, Potluri S, Surapaneni H, et al. Candidal infection of the gingiva mimicking desquamative gingivitis: A case report. Journal of Clinical and Diagnostic Research. 2016;10(3):ZD04–ZD05.
doi:10.7860/JCDR/2016/17413.7367
[4] da Silva MK, de Carvalho ACG, Alves EHP, et al. Genetic factors and the risk of periodontitis development: Findings from a systematic review composed of 13 studies of meta-analysis with 71,531 participants. International Journal of Dentistry. 2017;2017:1914073.
doi:10.1155/2017/1914073
[5] Jafri Z, Bhardwaj A, Sawai M, Sultan N. Influence of female sex hormones on periodontium: A case series. Journal of Natural Science, Biology and Medicine. 2015;6(Suppl1):S146–S149. doi:10.4103/0976-9668.166124
[6] Decker AM, Taichman LS, D’Silva NJ, Taichman RS. Periodontal treatment in cancer patients: An interdisciplinary approach. Current Oral Health Reports. 2018;5(1):7–12.
[7] Ababneh KT, Al-Omari M, Alawneh N. The effect of dental restoration type and material on periodontal health. Oral Health & Preventive Dentistry. 2011;9(4):395-403.
[8] Jagelavičienė E, Vaitkevičienė I, Šilingaitė D, et al. The relationship between Vitamin D and periodontal pathology. Medicina (Kaunas). 2018;54(3):45. doi:10.3390/medicina54030045
[9] Tappuni AR, Wilson N. Dry mouth: advice and management. The Pharmaceutical Journal. 2018. Retrieved from pharmaceutical-journal.com/article/ld/dry-mouth-advice-and-management
[10] Al-Bayaty FH, Baharuddin N, Abdulla MA, et al. The influence of cigarette smoking on gingival bleeding and serum concentrations of haptoglobin and alpha 1-antitrypsin. BioMed Research International. 2013.