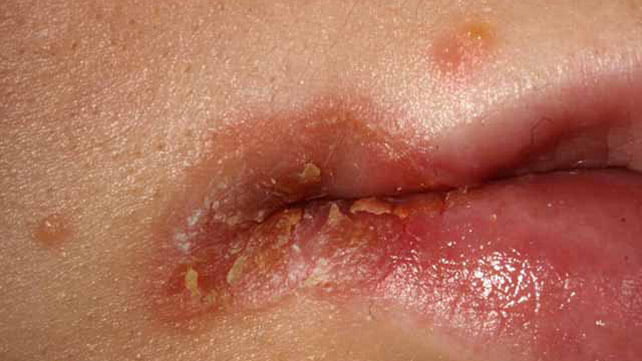
Angular Cheilitis is a condition which can cause red and swollen patches in the corners of your mouth where your lips meet and make an angle. This condition has other names such as angular stomatitis and perleche. You can get angular cheilitis on one side of your mouth or on the both sides at the same time. It is very common situation for people who have diabetes to get fungal infections like angular cheilitis. This is happening because the fungi like Candida feed off glucose, which is a blood sugar that our body is using as a source of energy. People, who have diabetes, have too much glucose in their blood. When there is an extra glucose, then this can create a breeding ground for fungus. Diabetes can also weaken our immune system which can make harder for us to fight off infection. When you keep your blood glucose levels in check, then this can help to prevent conditions like angular cheilitis. You should exercise, eat well and take your insulin correctly. Also it is very important for you not to smoke. Angular cheilitis is an inflammatory condition which can last a few days or it can be a chronic problem. This condition can affect people from all ages in which infants are also included. [1,2]
Symptoms of Angular cheilitis
The irritation and soreness in the corner or corners of your mouth are the main things which you will notice. The symptoms of this condition can be both cosmetically frustrating and physically painful. Also they can vary from having only mild redness to having open and bleeding blisters. If you are experiencing this condition, then the one or both corners of your mouth may be:
- Swollen
- Scaly
- Red
- Painful
- Itchy
- Crusty
- Cracked
- Blistered
- Bleeding
Also there are other symptoms of this condition which include:
- Difficulty eating as a result of the irritation
- Lips feeling dry or chapped
- Burning feeling on your lips or mouth
- Bad taste in your mouth
Your lips can feel uncomfortable and dry. Also there are some cases when you can feel that your mouth and lips are burning. Also you can have a bad taste in your mouth. If the irritation is strong, then this can make hard for you to eat. You may lose weight or you may not get enough nutrients. If you have noticed some of the mentioned symptoms of angular cheilitis, then you should talk with your doctor to determine how to treat it.

Risk factors of angular cheilitis
People who have corners of their mouth which are moist a lot of the time, are having increased risk of developing angular cheilitis. This can happen for many different reasons such as:
- You do not get enough nutrients, like iron or Vitamin B [3,5]
- You smoke [4]
- You suck your thumb
- You have sagging skin around your mouth from weight loss or age
- Your teeth are crooked, or you bite is not lined up correctly
- You have a lot of saliva
- You lick your lips a lot
- You have sensitive skin [5]
- You wear dentures that do not fit well [6]
- You have braces
There are some medical conditions which can increase your risk of getting angular cheilitis such as:
- Kidney, liver, lung or pancreatic cancer
- Immune disorders, like HIV
- Down syndrome
- Diabetes [1,2]
- Have other inflammatory illnesses, like Crohn’s disease
- Cancers of the blood
- Anemia
Causes: There are many different causes for angular cheilitis. The most common cause is the yeast infection as a result of saliva. Saliva gets trapped and it builds up in the corners of the mouth. When it dries, then the skin area can crack. Many people lick their lips often because this helps them to soothe their cracked skin. The moisture and warmth in the corners of the mouth are creating the perfect conditions for fungus to grow and multiply and they cause an infection. Also the second most common cause for the angular cheilitis is ther fungal infection. It is usually caused by a type of yeast which is called Candida which is the same fungus that is cause for diaper rash in babies. Also there are certain bacteria strains which can cause it. If your doctor cannot find the cause, then it is called idiopathic angular cheilitis. Bacteria and viruses can also cause angular cheilitis to develop. [7]
References:
[1] Rahmi, Argadianti AF, Radithia D, Soebadi B. Angular cheilitis in elderly patient with diabetes mellitus and decrease of vertical dimensions. Acta Medica Philippina. 2019;53(5):440-3.
[2] Sousa MGdM, Costa AdLL, Roncalli AG. Clinical study of the oral manifestations and related factors in type 2 diabetics patients. Brazilian Journal of Otorhinolaryngology. 2011;77(2):145-52.
[3] Zaidan TF. Angular cheilitis and iron deficiency anemia. MDJ. 2008;5:37-41.
[4] Ralho A, Coelho A, Ribeiro M, et al. Effects of electronic cigarettes on oral cavity: A systematic review. Journal of Evidence Based Dental Practice. 2019;19(4):101318.
[5] Oza N, Doshi JJ. Angular cheilitis: A clinical and microbial study. Indian Journal of Dental Research. 2017;28(6):661-5.
[6] Cross DL, Short L. Angular cheilitis occurring during orthodontic treatment. A case series. Journal of Orthodontics. 2009;35(4):229-33.
[7] Hellstein JW, Marek CL. Candidiasis: Red and white manifestations in the oral cavity. Head and Neck Pathology. 2019;13(1):25–32.