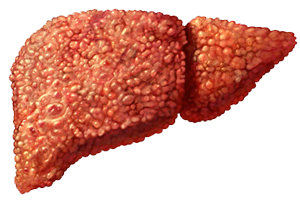
Cirrhosis is the late stage of fibrosis (scarring) of the liver. It can be caused by many forms of liver conditions and diseases such as chronic alcoholism and hepatitis. Our liver carries out several necessary functions such as detoxifying harmful substances in your body, cleaning your blood and making vital nutrients. This condition is happening in response to the damage to our liver. Each time when our liver is injured, it tries to repair itself. In this process scar tissue is forming. As this condition progresses, more and more scar tissue forms which is making it difficult for the liver to function. When there is development of specific complications which are resulting from the changes brought on by cirrhosis, then it is used the term – decompensated cirrhosis. The liver damage which is done by cirrhosis in the most cases cannot be undone. You need to go on regular checkups with your doctor because when the liver cirrhosis is diagnosed in the early stages and when the cause is treated, then further damage can be limited and in rarely cases it can be reversed. [1]
Symptoms of Cirrhosis
In the most cases cirrhosis does not have signs or symptoms until the liver damage is extensive. When the signs and symptoms occur, then they include:
- Breast enlargement in men
- Testicular atrophy in men
- Redness in the palms of the hands
- Spiderlike blood vessels on your skin
- Confusion, drowsiness and slurred speech (hepatic encephalopathy)
- Weight loss
- Swelling in your legs
- Nausea
- Loss of appetite
- Fluid accumulation in your abdomen (ascites)
- Yellow discoloration in the skin and eyes (jaundice)
- Itchy skin
- Bruising easily
- Bleeding easily
- Fatigue

If you have any of the signs and symptoms that are listed above, then you should visit your doctor as soon as possible.
Causes: There are many different diseases and conditions which can damage your liver and they can lead to cirrhosis. The most common causes for cirrhosis are:
- Fat accumulating in the liver (nonalcoholic fatty liver disease) [2]
- Chronic viral hepatitis (hepatitis B and C) [3]
- Chronic alcohol abuse [1]
Also there are other possible causes for cirrhosis such as
- Medications such as methotrexate [4]
- Infection such as schistosomiasis [5]
- Hardening and scarring of the bile ducts (primary sclerosing cholangitis) [6]
- Destruction of the bile ducts (primary biliary cirrhosis) [6]
- Liver disease caused by your body’s immune system (autoimmune hepatitis) [1]
- Genetic digestive disorder (Alagille syndrome) [7]
- Inherited disorders of sugar metabolism (galactosemia or glycogen storage disease)
- Poorly formed bile ducts (biliary atresia) [6]
- Copper accumulation in the liver (Wilson’s disease) [8]
- Cystic fibrosis [9]
- Iron buildup in the body (hemochromatosis)
Complications: Complications of cirrhosis can include:
- Complications related to blood flow:
- Bleeding: Portal hypertension can cause blood to be redirected to smaller veins which is causing them to increase in size and become varices. These smaller veins can burst because they are strained by the extra load and this can result in serious bleeding. Life – threatening bleeding most commonly occurs when veins in the stomach (gastric varices) and in the lower esophagus (esophageal varices) rupture. If your liver cannot make enough clotting factors, then this can also contribute to continued bleeding. Bacterial infections are the most frequent trigger for bleeding. [5]
- Enlargement of the spleen (splenomegaly): Portal hypertension can also cause changes to the spleen. If you have decreased white blood cells and platelets in your blood, then this can be a sign that you have cirrhosis with portal hypertension. [10]
- Swelling in the legs and abdomen: Portal hypertension can cause fluid to accumulate in the abdomen and legs. Ascites and edema can also result from the inability of your liver to make enough certain blood proteins such as albumin.
- High blood pressure in the veins that supply the liver (portal hypertension): Cirrhosis is slowing down the normal blood flow through the liver and it is increasing the pressure in the vein that brings blood from the intestines and spleen to liver.
- Other complications:
- Acute – on – chronic liver failure
- Increased risk of liver cancer
- Bone disease
- Jaundice
- Buildup of toxins in the brain (hepatic encephalopathy)
- Malnutrition
- Infections
References:
[1] Simpson RF, Hermon C, Liu B, et al. Alcohol drinking patterns and liver cirrhosis risk: analysis of the prospective UK Million Women Study. The Lancet: Public Health. 2018;4(1):E41-8.
[2] Green CJ, Hodson L. The influence of dietary fat on liver fat accumulation. Nutrients. 2014;6(11):5018–33.
[3] Iredale JP. Cirrhosis: new research provides a basis for rational and targeted treatments. BMJ. 2003;327(7407):143–7.
[4] Cheema E, Al-Aryan A, Al-Hamid A. Medicine use and medicine-related problems in patients with liver cirrhosis: a systematic review of quantitative and qualitative studies. European Journal of Clinical Pharmacology. 2019;75:1047-58.
[5] Bartoletti M, Giannella M, Lewis RE, Viale P. Bloodstream infections in patients with liver cirrhosis. Virulence. 2016;7(3):309–19.
[6] Vichido-Luna MA, Zarate-Mondragon F, Mora-Tiscareño MA, et al. Biliary cirrhosis secondary to bile duct obstruction by hamartomatous polyps in a patient with Peutz–Jeghers syndrome. Case Report. Gastroenterología y Hepatología. 2017;40(7):459-62.
[7] Scorza M, Elce A, Zarrilli F, et al. Genetic diseases that predispose to early liver cirrhosis. International Journal of Hepatology. 2014.
[8] Zhong HJ, Xiao P, Lin D, et al. Cirrhosis in Wilson disease is characterized by impaired hepatic synthesis, leukopenia and thrombocytopenia. International Journal of Medical Sciences. 2020;17(10):1345–50.
[9] Kamal N, Surana P, Koh C. Liver disease in patients with cystic fibrosis. Current Opinion in Gastroenterology. 2018;34(3):146–51.
[10] Li L, Duan M, Chen W, et al. The spleen in liver cirrhosis: revisiting an old enemy with novel targets. Journal of Translational Medicine. 2017;15:111.