The overactive bladder is also known as OAB. It is causing a frequent and sudden urge to urinate that may be difficult to control. You may feel that you need to pass urine many times during the day and night. Also, you may experience unintentional loss of urine (also known as urinary incontinence). If you have an overactive bladder and you feel embarrassed, then isolate yourself or limit social life and work. But, there is good news for you.
A brief evaluation can determine whether there is a specific cause for your overactive bladder symptoms. You may be able to regulate the symptoms of overactive bladder with simple behavioral strategies, such as timed voiding, dietary changes, and bladder–holding techniques using your pelvic floor muscles. If these initial efforts do not help enough with the overactive bladder symptoms, then additional treatments are available.
Overactive Bladder: Symptoms
If you have an overactive bladder, then you may:
- Wake up more than 2 times in the night to urinate (which is also known as nocturia)
- Urinate frequently, usually 8 or more times in 24 hours
- Experience unintentional loss of urine immediately after an urgent need to urinate (this is also known as urgency incontinence)
- Feel an immediate urge to urinate that is difficult to control
Even if you are able to get to the toilet at the time when you have an urge to urinate, nighttime urination and unexpected frequent urination can disrupt your life. Overactive bladder is very common among older adults, but it is not a normal part of aging. [1,2] It may not be easy for you to discuss your symptoms with your doctor, but if they are disrupting or distressing your life, then you should talk with your doctor as soon as possible. There are many different types of treatments for overactive bladder which can help you to feel better.
Causes:
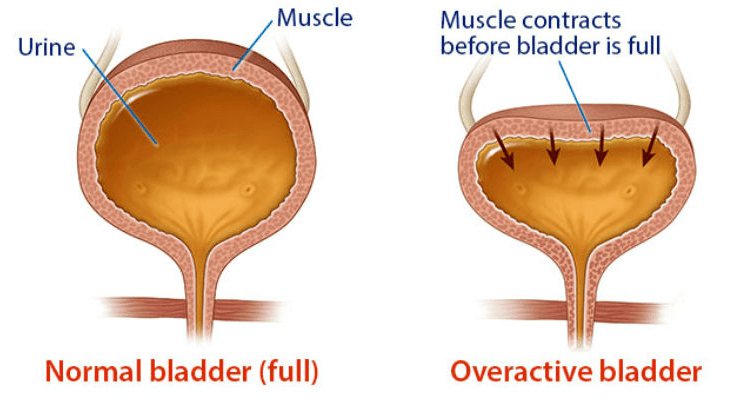
- Normal bladder function: Our kidneys produce urine which drains into the bladder. When you urinate, the urine is passing from your bladder through a tube called the urethra. The muscle in the urethra known as the sphincter opens to release the urine out of the body. In women, the urethral opening is located just above the vaginal opening while in men the urethral opening is at the tip of the penis. As your bladder fills, the nerve signals sent to your brain eventually trigger the need to urinate. When you urinate, then those nerve signals coordinate the relaxation of the pelvic floor muscles and the muscles of the urethra (which are known as urinary sphincter muscles). The muscles of the bladder tighten or contract, pushing the urine out.
- Involuntary bladder contractions: The overactive bladder happens because the muscles of the bladder start to contract involuntarily even when the volume of the urine in the bladder is low. These involuntary contractions are creating an urgent need to urinate. There are several conditions that may contribute to the signs and symptoms of overactive bladder, such as
- Some factors that obstruct bladder outflow – enlarged prostate, constipation, or previous operations to treat other forms of incontinence [2]
- Certain abnormalities in the bladder, such as tumors or bladder stones
- Hormonal changes during menopause in women [3]
- Urinary tract infections that can cause symptoms similar to those of an overactive bladder
- Diabetes [4]
- Some neurological disorders, such as stroke and multiple sclerosis [5]
Also, there can be other factors that may be associated with your symptoms, such as
- An incomplete bladder emptying, which may lead to symptoms of the overactive bladder as you have little urine storage space left
- A difficulty in walking, which can lead to bladder urgency if you are unable to get to the bathroom quickly
- A declining cognitive function due to aging, which may make it more difficult for your bladder to understand the signals it receives from your brain [1,2]
- Excess consumption of caffeine or alcohol [6,7]
- Some medications that cause a rapid increase in urine production or require that you take them with lots of fluids
Risk factors: Some risk factors for overactive bladder include:
- Age [1,2]
- Enlarged prostate
- Diabetes [4]
- Cognitive decline [8]
References:
[1] Wolff GF, Kuchel GA, Smith PP. Overactive bladder in the vulnerable elderly. Research and Reports in Urology. 2014;6:131–8. doi:10.2147/RRU.S41843
[2] Shah D, Badlani G. Treatment of overactive bladder and incontinence in the elderly. Reviews in Urology. 2002;4(Suppl4):S38–S43.
[3] Zhu L, Cheng X, Sun J, et al. Association between menopausal symptoms and overactive bladder: A cross-sectional questionnaire survey in China. Plos One. 2015.
[4] Golbidi S, Laher I. Bladder dysfunction in diabetes mellitus. Frontiers in Pharmacology. 2010;1:136. doi:10.3389/fphar.2010.00136
[5] Pyo H, Kim BR, Park M, et al. Effects of overactive bladder symptoms in stroke patients’ health related quality of life and their performance scale. Annals of Rehabilitation Medicine. 2017;41(6):935–43. doi:10.5535/arm.2017.41.6.935
[6] Lohsiriwat S, Hirunsai M, Chaiyaprasithi B. Effect of caffeine on bladder function in patients with overactive bladder symptoms. Urology Annals. 2011;3(1):14–18. doi:10.4103/0974-7796.75862
[7] Zhu J, Hu X, Dong X, Li L. Associations between risk factors and overactive bladder: A meta-analysis. Female Pelvic Medicine & Reconstructive Surgery. 2019;25(3):238-46.
doi:10.1097/SPV.0000000000000531
[8] Jung HB, Choi DK, Lee SH, et al. Correlation between overactive bladder symptom score and neuropsychological parameters in Alzheimer’s disease patients with lower urinary tract symptom. International Brazilian Journal of Urology. 2017;43(2):256–63.
doi:10.1590/S1677-5538.IBJU.2015.0664